Rhythmical Massage Therapy in Chronic Disease: A 4-Year
Prospective Cohort Study
HARALD J. HAMRE, M.D., 1 CLAUDIA M. WITT, M.D., 2 ANJA GLOCKMANN, Dipl.Biol., 1 RENATUS ZIEGLER, Ph.D., 3 STEFAN N. WILLICH, M.D., M.P.H., 2 and HELMUT KIENE, M.D.
1 Institute for Applied Epistemology and Medical Methodology,
Freiburg, Germany.
2 Institute for Social Medicine, Epidemiology, and Health
Economics, Charite University Medical
Center, Berlin, Germany.
3 Society for Cancer Research, Arlesheim, Switzerland.
ABSTRACT
Objective: Rhythmical massage therapy is used in 24
countries but has not yet been studied in outpatient settings. The objective
was to study clinical outcomes in patients receiving rhythmical massage therapy
for chronic diseases.
Design: Prospective 4-year cohort study.
Setting: Thirty-six (36) medical practices in Germany.
Participants: Eighty-five (85) outpatients referred to
rhythmical massage therapy.
Outcome measures: Disease and Symptom Scores (physicians'
and patients' assessment, respectively, 0-10) and SF-36. Disease Score was
measured after 6 and 12 months, and other outcomes after 3, 6, 12, 18, 24, and
48 months.
Results: Most common indications were musculoskeletal
diseases (45% of patients; primarily back and neck pain) and mental disorders
(18%, primarily depression and fatigue). Median disease duration at baseline
was 2.0 years (interquartile range 0.5-6.0). Median number of rhythmical massage
therapy sessions was 12 (interquartile range 9-12), and median therapy
duration was 84 (49-119) days. All outcomes improved significantly between
baseline and all subsequent follow-ups. From baseline to 12 months, Disease
Score improved from (mean plus or minus standard deviation) 6.30 ± 2.01 to 2.77
plus or minus 1.97 (p < 0.001), Symptom Score improved from 5.76 ± 1.81 to
3.13 ± 2.20 (p < 0.001), SF-36 Physical Component score improved from 39.55
± 9.91 to 45.17 ± 9.88 (p < 0.001), and SF-36 Mental Component score
improved from 39.27 ± 13.61 to 43.78 ± 12.32 (p = 0.028). All these
improvements were maintained until the last follow-up. Adverse reactions to
rhythmical massage therapy occurred in 4 (5%) patients; 2 patients stopped
therapy because of adverse reactions.
Conclusions: Patients receiving rhythmical massage therapy had long-term reduction of chronic disease symptoms and improvement of quality
of life.
INTRODUCTION
Anthroposophic medicine (AM) was founded by Rudolf Steiner,
Ph.D., Free Academy of Spiritual Science, Dornach, Switzerland, and Ita
Wegman, M.D., Free Academy of Spiritual Science, and Clinical Therapeutic
Institute, Arlesheim, Switzerland.1 AM
extends conventional medicine through a holistic approach to humans and nature,
addressing physical, psychologic, and spiritual aspects of the patients (Table
1) 2,3 AM is provided by physicians (counseling, AM medication) and nonmedical
therapists (art therapy, eurythmy movement exercises, and rhythmical massage
therapy [RMT]).2
RMT was developed from Swedish massage by Dr. Wegman, a
physician and physiotherapist.4 Special RMT techniques include lifting
movements, rhythmically undulating gliding movements, and complex movement
patterns such as lemniscates (Table 1). In addition to effects on the skin,
subcutaneous tissues, and muscles, RMT is believed to have both general effects
(e.g., enhancing physical vitality) and disease-specific effects (Table 1). RMT
can be used as monotherapy or in conjunction with other therapies. RMT is
practiced by physiotherapists with additional 11/2-3 years of RMT training
according to a standardized curriculum. RMT schools exist in Australia, Germany,
Italy, South Africa, Switzerland,
and the United States.
Presently, RMT is provided by approximately 700 therapists in 24 countries
worldwide (U. Niedermann, International Coordination AM, personal
communication, May 2007).
Observational studies in inpatient settings suggest that RMT
can have clinically relevant effects 3,5,6 However, these studies evaluated
several AM therapies, and only a proportion of the patients received RMT. Here
we present a long-term study of RMT users.
TABLE 1. DESCRIPTION of RHYTHMICAL MASSAGE THERAPY (RMT)
Postulated working principles
According to the anthroposphic understanding of humans and
nature, four different classes
of formative forces can be discerned: (1) in minerals, material forces of
physico-chemical matter; (2) in plants, formative vegetative forces interact
with material forces, bringing about and maintaining the living form; (3) in
animals with sensory and motor systems and with a corresponding inner life, a
further class of formative forces (anima, soul) interacts with material and
vegetative forces; (4) in the human organism with its individual mind and
capacity of thinking, another class of formative forces (Geist, spirit)
interacts with the material, vegetative, and mineral forces. The interactions
of these forces are understood to vary between different regions and organs in
the human body, resulting in a complex equilibrium. This equilibrium can be
distorted in various forms of human disease, and is sought to be regulated by
RMT and other anthroposophic therapies.
Indications
RMT is used for a wide range of indications in family
practice, internal medicine, surgery, orthopedics, neurology, gynecology,
pediatrics, geriatrics, psychiatry, and rehabilitation.
Contraindications
Cancer (nonremitted or not radically operated), acute
infections, acute eczema, pregnancy.
Overall structure of therapy
First 1-2 sessions are primarily diagnostic, gathering
verbal, visual, and tactile information from the patient: body proportions and
posture, quality of skin and soft tissues, muscle tone, warmth distribution,
respiration, sensitivity to touch. Remaining sessions are primarily
therapeutic.
Use of conversation
First 1-2 sessions: extensive. Remaining sessions: initial
brief conversation only.
Use of music
No.
Lubricants
Vegetable oils, used sparingly.
Body areas massaged
In general, RMT of the arms or upper back aims to intensify
the involvement of soul and spirit forces with material and vegetative forces,
whereas massage of the lower limbs aims to weaken this involvement. Therapists
may also work on one part of the body to create an effect in another part.
Special massage programs (each with specified patient position, sequence of
techniques, movement patterns, and duration of treatment) exist for the hands,
arms, anterior and posterior lower limbs, feet, knees, hips, lower back, whole
back, neck, abdomen, and head.
Supplementary organ treatment
Optionally, an ointment containing metals such as copper or
iron is lightly rubbed into the skin near a major organ (liver, kidneys, heart,
or spleen) to stimulate, calm, or harmonize organ function. Duration of
treatment 1-2 min.
Massage techniques
Effeurage (gliding) with light, rhythmically undulating
pressure, keeping therapist's palm in good contact with patient's skin.
Kneading with circular, loop-shaped movements. Gentle lifting movements with
both hands. Friction. Percussion. Vibration.
Movement direction
Differentiation: e.g., massaging the legs upwards can create
a greater sense of vitality and "awakeness"; working with the legs
downwards is used to "anchor" patients back into their bodies.
Special movement patterns
Circle: single or double, i.e., performed with reciprocal
phase-displaced movements of both hands. Spiral: single (e.g., for abdomen,
liver, knee, or knuckle) or moving upward (e.g., posterior thigh, upper back).
Spiral + circle (soothing heart treatment). Lemniscate = figure of eight: fixed
(stimulating heart treatment) or moving upwards (whole back). Lemniscate forms
can be symmetric (lower ack), have different size of the two circles (spleen),
or asymmetric crossing of the circles (kidney). Zig-zag: downward (abdomen).
Centripetal (lower back, forehead).
Temperature
Throughout the massage the patient is kept warm, with only
the massaged parts of the body exposed. Windows are closed; draughts are
avoided. Mild hot packs may be applied.
Rest period after massage
Considered essential to achieve desired effects. The patient
is wrapped in towels and blankets and left in a darkened room.
Duration of treatment
Massage: usually 20-30 min. Rest period: at least 20 min.
Frequency of therapy sessions
Once or twice weekly.
Number of sessions
Usually 6-12 sessions.
Supplementary advice and information
Lifestyle changes (e.g. diet, alcohol, or smoking
restriction, exercises), footbaths or limb washes with particular oils may be
recommended.
Table structure adapted from Goldstone LA. Massage as an orthodox
medical treatment past and future. Complement Ther Nurs Midwifery
2000;6:169-175. Description condensed from refs. 1-4. Also from Glockler M,
Schurholz J, Treichler M. Anthroposophic Medicine [in German]. In: Zentrum zur
Documentation fin Naturheilverfahren e.V., Forschungsinstitut Freie Berufe,
eds. Documentation of Special and Naturopathic Therapy Systems in Europe [in German]. Essen:
VGM-Verlag, 1991:214-335.
MATERIALS AND METHODS
Study design and objective
This prospective cohort study was part of a research project
on the effectiveness and costs of AM therapies in outpatients with chronic
disease (Anthroposophic Medicine Outcomes Study, AMOS).7,8 The AMOS project was
initiated by a health insurance company in conjunction with a health benefit
program. The present study assessed symptoms, quality of life, adjunctive
therapies, adverse reactions, and therapy satisfaction in outpatients receiving
RMT under routine clinical conditions.
Setting and participants
All physicians certified by the Physicians' Association for
Anthroposophical Medicine in Germany
and treating outpatients in Germany
were invited to participate. The participating physicians were instructed to
recruit consecutive outpatients ages 1-75, referred to RMT for any indication
(main diagnosis). Exclusion criteria were previous RMT for main diagnosis, or
ongoing RMT. RMT therapists were certified by the German Rhythmical Massage
Therapy Association. RMT was implemented according to the RMT therapists'
discretion. Other therapies such as AM medication, AM art or eurythmy
exercises, or non-AM adjunctive therapies were allowed throughout the study.
Participating physicians (n = 36) did not differ significantly
from all AM-certified physicians in Germany (n 362) regarding gender (56%
versus 62% males), age (mean standard deviation 47.3 ± 7.2 versus 47.5 ± 7.9
years), number of years in practice (19.3 ± 7.6 versus 19.5 ± 8.7), and the
proportion of primary care physicians (94% versus 85%). Participating
therapists (n = 33) did not differ from RMT therapists without study patients
(n = 122) regarding gender (76% versus 74% females), age (mean 50.1 ± 7.2 versus 50.0 ± 9.7 years), or number of years since RMT certification
(mean 7.7 ± 2.0 versus 7.4 ± 3.7 years).
Clinical outcomes
Since the study encompassed different diagnoses, disease
severity was assessed uniformly for all diagnoses on numerical scales from 0
("not present") to 10 ("worst possible"):
Disease Score (physician's assessment of severity of main diagnosis);
Symptom Score (patients' assessment of one to six most relevant symptoms
present at baseline). In patients greater or equal to age 17 years, quality of
life was assessed with a widely used generic instrument, the SF (Short Form)-36
Health Survey: Physical and Mental Component Summary Measures, the eight SF-36
scales, and the SF-36 Health Change item.9 Disease Score was documented after
0, 6, and 12 months, Symptom Score and SF-36 after 0, 3, 6, 12, 18, 24, and 48
months.
Other outcomes
- Adjunctive
therapy use
- Therapy
ratings
- Adverse reactions (physician and patient documentation).
Data collection
All data were documented with questionnaires sent in sealed
envelopes to the study office. Physicians documented eligibility criteria;
therapists documented RMT administration; remaining items were documented by
patients/caregivers, unless otherwise stated. Patient responses were not made
available to physicians. Physicians were compensated40 Euro (US $55) per patient, patients received no compensation.
Quality assurance and adherence to regulations
The study was approved by the Ethics Committee of the Faculty
of Medicine Charite, Humboldt University Berlin, and was conducted according to
the Helsinki Declaration and the International Conference on Harmonisation—Good
Clinical Practice Guidelines. Written informed consent was obtained from all
patients before enrollment.
Data analysis
Data analysis (SPSS® 13.0.1 [SPSS, Inc., Chicago,
IL] and StatXact® 5.0.3 [CyteI Software
Corporation, Cambridge, MA]) was performed on all patients
fulfilling eligibility criteria. The two-tailed t-test was used for continuous
data, two-tailed McNemar test and Fisher's exact test for dichotomous data. Significance criteria were p < 0.05 and 95% confidence interval not including 0. Because this was a
descriptive study, no adjustment for multiple comparisons was performed.10
Pre-post effect sizes were calculated as Standardized Response Mean and
classified as small (0.20-0.49), medium (0.50-0.79), and large ( >0.80). 11
RESULTS
Patient recruitment and follow-up
From July 1, 1998 to March 31, 2001, a total of 85 patients
were included in the study (Fig. 1). 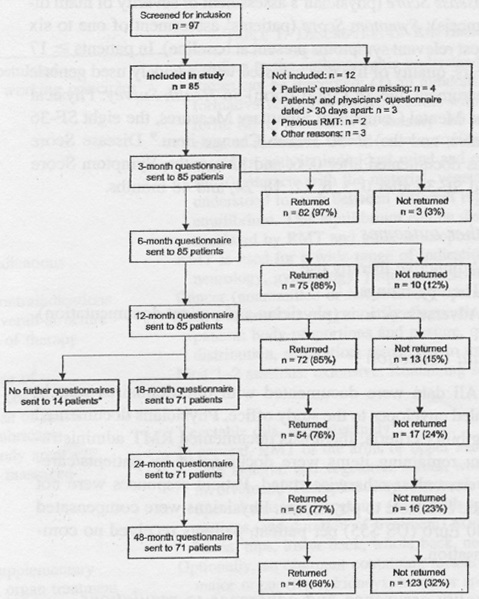
FIG. 1. Patient recruitment and follow-up. *18-, 24-, and 48-month follow-up questionnaires were not sent to patients enrolled before January 1, 1999.
The last patient follow-up ensued March
30, 2005. Ninety-six percent (96%)(82/85) of patients returned at least one follow-up questionnaire.
Respondents and nonrespondents of the 12-month questionnaire did not differ
significantly regarding gender, main diagnosis, duration of main diagnosis,
baseline Disease Score, or baseline Symptom Score. Median age was 19.0 (interquartile
range [IQR] 8.0-37.5) years in nonrespondents and 37.5 (29.5-50.8) years in
respondents (p = 0.009).
The total number of patients referred to RMT during the
study was estimated by the physicians (response rate 64%, 23/36 physicians).
The proportion of referred versus enrolled patients was median 6.6 (IQR
1.8-12.4). There was no significant correlation between this proportion and the
0-12-month improvement of Symptom Score (Spearman-Rho 0. 10, p = 0.524, n = 44
patients).
Baseline characteristics
Patients were recruited from 12 of 16 German federal states.
Median age was 37.0 years (IQR 20.5-48.0, mean 35.7 ± 19.3 years), and 76%
(65/85) of patients were women. Physicians' setting was primary care practice
(95% of patients, n = 81/85), referral practice (1%), and outpatient clinic
(4%).
Most frequent main diagnoses, classified by ICD-10 (International
Classification of Diseases, Tenth Edition), were M00—M99 Musculoskeletal
Diseases (45%, n = 38/85 patients), F00—F99 Mental Disorders (18%), and
G00—G99 Nervous System Disorders (8%). Most frequent single diagnoses were
back and neck pain (32%, n = 27/85 patients), depression/fatigue (8%),
headache/migraine (7%), and fibromyalgia (5%). Median duration of main
diagnosis was 2.0 years (IQR 0.5-6.0, mean 5.2 ± 7.8 years).
Patients had median 2.0 (IQR 1.0-3.0) comorbid diseases.
Most common comorbid diseases were F00—F99 Mental Disorders (20%, 27/137
diagnoses), M00—M99 Musculoskeletal Diseases (15%), and 100-199 Circulatory
Diseases (12%).
Therapies
RMT administration was documented during the first 24 months
after study enrollment. In this period 91% (77/85) of patients had RMT; for 9%
RMT documentation is incomplete. RMT started a median of 7 (IQR 0-18) days after
enrollment. Median therapy duration was 84 (IQR 49-119) days, and the median
number of RMT sessions was 12 (9-12). During the first 6 study months, 76%
(65/85) of patients used AM medication, 14% (12/85) had AM eurythmy therapy, and
2% (2/85) had AM art therapy.
Use of diagnosis-related adjunctive therapies within the
first 6 study months was analyzed in patients with a main diagnosis of
musculoskeletal or mental diseases or headache disorders (n = 59, Table 2). Of
51 evaluable patients, 47% (n = 24) had no diagnosis-related adjunctive
therapy.

Clinical outcomes
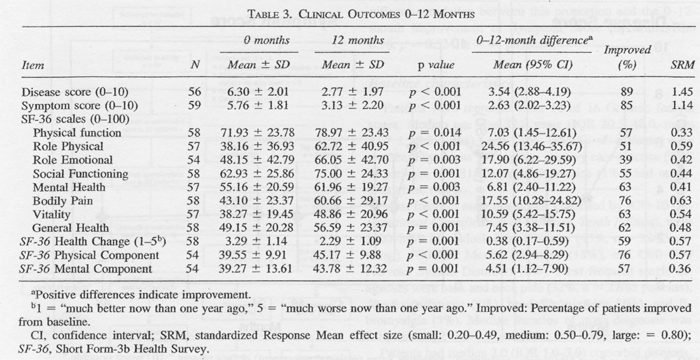
Disease and Symptom Scores (Fig. 2) and the 11 SF-36 scores
(Fig. 3) improved significantly between baseline and most subsequent
follow-tips (69 significant and 5 nonsignificant improvements in 74 pre—post
comparisons). Most improvements occurred during the first 6 months. After 12
months, Disease and Symptom scores were improved from baseline in 89% and 85%
of patients, respectively (Table 3); an improvement of 30% (or better) of
baseline scores was observed in 82% (46/56) and 64% (38/59) of evaluable
patients, respectively. Disease and Symptom Scores improved similarly in
adults and in children. Effect sizes for the 0-12-month comparison were large
for Disease and Symptom Scores (IA5 and 1.14) and small-to-medium (range
0.33-0.63) for SF-36 scores. All these improvements were maintained until the
last follow-up.

FIG. 2. Disease Score (physicians' assessment), Symptom Score (patients' assessment), 0 "not present," 10 "worst possible."
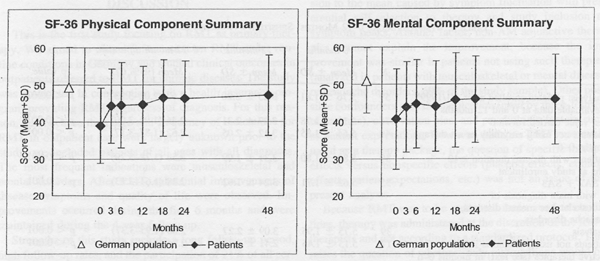
FIG. 3. SF (Short Form)-36 Physical and Mental Component Summary Measures. Higher scores indicate better health. Adult patients and German population (age 17-74 years).9
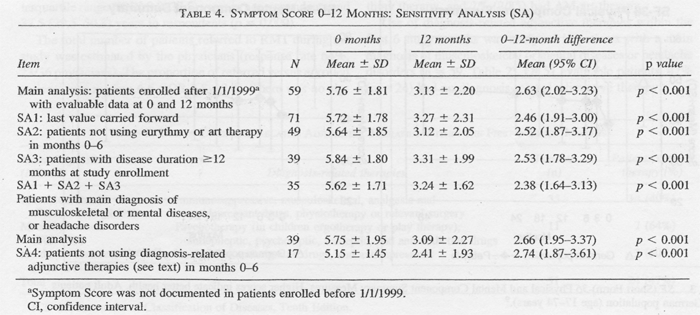 In order to test the influence of four bias factors on
0-12-month Symptom Score outcomes, we performed post hoc sensitivity analyses
(Table 4). The first sensitivity analysis (SAI) concerned dropout bias. The
main analysis had comprised all patients with evaluable data at baseline and
12-month follow-up. In SAI, missing values after 12 months were replaced with
the last value carried forward, reducing the average 0-12-month improvement by
6% (2.63 ---> 2.46 points). SA2 concerned the effect of AM adjunctive
therapies: The sample was restricted to patients using neither eurythmy nor art
therapy in the first 6 study months, reducing the improvement by 4% (2.63 ->
2.52 points).
In order to test the influence of four bias factors on
0-12-month Symptom Score outcomes, we performed post hoc sensitivity analyses
(Table 4). The first sensitivity analysis (SAI) concerned dropout bias. The
main analysis had comprised all patients with evaluable data at baseline and
12-month follow-up. In SAI, missing values after 12 months were replaced with
the last value carried forward, reducing the average 0-12-month improvement by
6% (2.63 ---> 2.46 points). SA2 concerned the effect of AM adjunctive
therapies: The sample was restricted to patients using neither eurythmy nor art
therapy in the first 6 study months, reducing the improvement by 4% (2.63 ->
2.52 points).
SA3 concerned spontaneous improvement, which was assumed to
be improbable in patients with disease duration 12 months: The sample was
restricted to patients with disease duration of >12 months prior to study
enrollment, reducing the improvement by 4% (2.63 2.53 points).
Combining SAI + SA2 + SA3, the improvement was reduced by a
total of 10%.
SA4 concerned the effects of relevant non-AM adjunctive
therapies, and was performed on patients with a main diagnosis of
musculoskeletal or mental diseases or headache disorders. Restricting this sample
to patients not using diagnosis-related adjunctive therapies during the first 6
study months (Table 2), the average Symptom Score improvement was increased by
3% (2.66 ---> 2.74 points).
Other outcomes
Therapy ratings: At 6-month follow-up, patients' average
therapy outcome rating (from 0 "no help at all" to 10 "helped
very well") was 7.50 ± 2.34; patient satisfaction with therapy (from 0
"very dissatisfied" to 10 "very satisfied") was 8.18 ±
2.08. Patients' RMT effectiveness rating was positive ("very
effective" or "effective") in 83% (57/69) of patients, and
negative ("less effective," "ineffective," or "not
evaluable") in 17%. Physicians' effectiveness rating was positive in 77%
(53/69) and negative in 23%. Ratings of therapy outcome, satisfaction, and
effectiveness did not differ significantly between adults and children, or
between 6- and 12-month follow-ups.
Adverse reactions during the first 24 study months: Adverse
reactions to RMT occurred in four (5%) patients: (1) mild cardiac palpitations;
(2) moderate arterial hypotension; (3) moderate pain and vertigo; and (4)
moderate (patient report)/severe (physician report) symptom aggravation. Patients
3 and 4 stopped RMT because of adverse reactions. No adverse reactions to AM
eurythmy or art therapy occurred. Adverse reactions to AM medications occurred
in 6% (4/70 users); adverse reactions to non-AM medication occurred in 11%
(8/74 users) (p = 0.369).
Serious adverse events. One patient died of breast cancer 22
months after study enrollment; this event had no relation to any therapy or
medication.
DISCUSSION
This is the first study focusing on RMT as primary therapy.
We aimed to obtain information on RMT under routine conditions in Germany and
studied clinical outcomes in outpatients referred to RMT for chronic diseases.
The study was conducted in conjunction with a health insurance program
providing RMT regardless of diagnosis. For this reason, and because the range
and frequency of indications for RMT in outpatient care were largely unknown
prior to the study, we included patients of all ages with all diagnoses. The
most frequent indications were musculoskeletal and mental disorders. After RMT,
substantial improvements of disease symptoms and quality of life were observed.
Improvements occurred during the first 6 months and were maintained during the
4-year follow-up.
Strengths of this study include a long follow-up period,
high follow-up rates, and the participation of 21% of all certified RMT
therapists in Germany.
Participants resembled all eligible therapists with respect to sociodemographic
characteristics. These features suggest that the study to a high degree mirrors
contemporary RMT practice.
Nevertheless, because the study had a long recruitment
period, the participating physicians were not able to screen and include all
patients referred to RMT. It was estimated that physicians enrolled 15% of such
patients. Selection bias could be present if physicians would preferentially
screen and enroll patients for whom a particularly positive outcome was
expected. In this case, one would expect the degree of selection (= the
proportion of referred versus enrolled patients) to correlate positively with
clinical outcomes. That was not the case, the correlation was almost zero
(0.10) and not significant. This analysis does not suggest that physicians'
screening of patients referred to RMT was affected by selection bias.
Because 13 clinical outcomes were analyzed, the issue of
multiple hypothesis-testing arises.10 However, all analyzed 0-12-month
comparisons of clinical outcomes showed significant improvements (Table 3),
and 11 of these 13 comparisons had p values less than or equal to 0.005.
Because patients with all diagnoses were included, our study
offers a comprehensive picture of RMT practice. On the other hand, it was not
feasible to have disease-specific outcomes for all diagnoses included.
Nonetheless, this study is part of a larger AM evaluation project that included
disease-specific outcomes for major disease groups. 12,13
A limitation of the study is the absence of a comparison group
receiving another treatment or no therapy. For the observed improvements, one
has to consider several other causes apart from RMT. Therefore, sensitivity
analyses were conducted in regard to dropout bias, adjunctive AM eurythmy or
art therapy, and spontaneous improvement. According to the analyses, these
three factors can together explain maximum 10% of the average 0-12-month improvement.
Notably, this analysis does not exclude regression to the mean caused by
symptom fluctuation with preferential self-selection to therapy and study
inclusion at symptom peaks. Another factor, non-AM adjunctive therapies,
cannot explain the improvement, because the improvement was similar in
patients not using such therapies (analyzed in patients with musculoskeletal or
mental disease or headache disorders, 69% of the study sample). Other possible
confounders are AM medication (used by three-fourths of patients), observation
bias, and psychologic factors such as patient expectations. However, because
RMT was evaluated as a therapy package, the question of specific therapy
effects versus nonspecific effects (placebo effects, context effects, patient
expectations, etc.) was not an issue of the present analysis.
Because RMT was to be evaluated under routine conditions,
therapy was administered at the discretion of the RMT therapists and not
according to a standardized protocol. This raises the question of whether study
interventions would be replicable in future studies. However, RMT therapists
worldwide are taught the same set of RMT techniques according to a highly
standardized curriculum. Therefore, relevant therapy differences across
settings would not be expected. Moreover, in this study, any local therapy
differences would probably be offset by the relatively large number of
participating RMT therapists.
Previous studies have evaluated AM therapy including RMT in
inpatient settings and found improved quality of life in breast cancer
patients;5 improved coping with chronic musculoskeletal pain;6 high anorexia
nervosa cure rates;3 and reduced pain, reduced medication use, and earlier
return to work in lumbar disc disease.3 In accordance with these findings, our
primary care study of patients with predominantly musculoskeletal and mental diseases
demonstrated longstanding clinically relevant improvements in disease symptoms
and quality of life. At 12-month follow-up, two-thirds of the patients had a
clinically relevant symptom improvement of at least 30% of their baseline
score. Altogether, the positive outcome of RMT in this study is encouraging.
CONCLUSIONS
In this first study focusing on RMT, patients treated with
RMT had substantial long-term reduction of chronic disease symptoms and
improvement of quality of life.
ACKNOWLEDGMENTS
This study was funded by the Software-AG Stiftung and the
Innungskrankenkasse Hamburg.
REFERENCES
1. Steiner R. Wegman I. Extending practical medicine. Fundamental
principles based on the science of the spirit. GA 27. Bristol: Rudolf Steiner Press, 2000, 144 p.
2. Ritchie J, Wilkinson J, Gantlet' M, et al. A model of
integrated primary care: Anthroposophic medicine. London. Department of General Practice and
Primary Care, St. Bartholomew's and the Royal London School of Medicine and
Dentistry, Queen Mary University of London, 2001.
3. Kienle GS, Kienle H, Albonico HU. Anthroposophic
medicine: Effectiveness, utility, costs, safety. Stuttgart, New York:
Schattauer Verlag, 2006, 336 p.
4. Hauschka-Stavenhagen M. Rhythmical Massage as Indicated
by Dr. Ita Wegman. Spring Valley,
NY: Mercury Press, 1990, 138 p.
5. Carlsson M, Arman M, Backman M, et al. Evaluation of quality
of life/life satisfaction in women with breast cancer in complementary and
conventional care. Acta Oncol 2004;43:27-34.
6. Flatters U, Arman M, Ekenback K. Pain rehabilitation in
the Vidar Clinic: Report of a project at the Vidar Clinic in collaboration
with Scania Partner AB and the Swedish Social Insurance Administration in Stockholm, 1988. Jarna:
Vidarkliniken, 1998, 24 p.
7. Hamre HJ, Becker-Witt C, Glockmann A, et al. Anthroposophic
therapies in chronic disease: The Anthroposophic Medicine Outcomes Study
(AMOS). Eur J Med Res 2004; 9:351-360.
8. Hamm HJ, Witt CM, Glockmann A, et al. Health costs in anthroposophic
therapy users: A two-year prospective cohort study. BMC Health Sery Res
2006;6:doi: 10. 1186/1472-6963-6-65.
9. Bollinger M, Kirchberger
I. SF-36 Health Survey, German Version:
Handbook. Gottingen:
Hogrefe-Verlag, 1998, 155 p.
10. Feise RJ. Do multiple outcome measures require p-value
adjustment? BMC Med Res Methodol 2002;2:8.
11. Liang MH, Fossel AH, Larson MG. Comparisons of five
health status instruments for orthopedic evaluation. Med Care 1990;28:632-642.
12. Hamre HJ, Witt CM, Glockmann A, et al. Anthroposophic
therapy for chronic depression: A four-year prospective cohort study. BMC
Psychiatry 2006;6:doi:10.1186/1471– 244X-6-57.
13. Hamre HJ, Witt CM, Glockmann A, et al. Anthroposophic
vs. conventional therapy for chronic low back pain: A prospective
non-randomised comparative study. Eur J Med Res 2007;12:1-9,
Address reprint requests to:
Harald J. Hamre, M.D.
Institute for Applied Epistemology
and Medical Methodology
Abteilung fur Klinische Forschung
Bocklerstrabe 5
D-79110 Freiburg, Germany
E-mail: harald.hamre@ifaemm.de
THE JOURNAL OF ALTERNATIVE AND COMPLEMENTARY MEDICINE
Volume 13, Number 6, 2007, pp. 635-642
copyright Mary Ann Liebert, Inc.
DOI: 10.1089/acm.2006.6345